



 back to Dr. Reid's Corner Directory
back to Dr. Reid's Corner DirectoryThe OptiFlowBC System: Combined Modality Treatment using the ReidSleeve® and the BioCompression Pneumatic Pump
 email this to a friend
email this to a friend
Authors:
Renee Robinson, Suzie Willis, Cheri Hoskins, Stephen Morgan, Ann Hafner and Tony Reid MD, Ph.D.
Duke University School of Medicine, Healthtronix Lymphedema Management, Inc. and Peninsula BioMedical, Inc.
Abstract
Patients - 35 patients (16 upper extremity/19 lower extremity) with refractory lymphedema were enrolled on a study using the Reid Sleeve in combination with the BioCompression/Optiflow system.
Methods - Patients wore the Reid Sleeve at night. During the daytime, the patients used the BioCompression pump with the Reid Sleeve Optiflow insert for 2 sessions of 60 minutes. Circumferential measurements were made at 3-inch intervals along the length of the arm or leg. The unaffected limb was used as control to determine the percent change from expected except when both limbs were effected.
Results - Among patients with upper extremity edema, the reduction in lymphedema increased steadily during treatment and was 24.7, 53.8 and 80.2% at 4, 12 and 28 weeks. The volume reduction at these times was 2310, 2753 and 4047 cubic centimeters. Linear regression analysis demonstrates a highly significant (p<0.001) reduction in arm edema during the course of treatment. A plateau phase occurred between weeks 4 and 8. For the patients with leg edema, the average reduction at 4 weeks was 9143 cubic centimeters followed by a period of relatively stable lymphedema until week 12 with an average decrease in lymphedema of 1486 cubic centimeters between weeks 12 and 16. Linear regression analysis demonstrates a significant (p<0.02) decrease in leg edema. The plateau phase may represent a tissue repair phase that occurs with effective resolution of residual lymphedema. Subsequent reductions in lymphedema can occur following tissue healing. The plateau phase appears to be more protracted among patients with more serious lymphedema such as patients with leg edema.
Background
Lymphedema is a chronic process due to lymphatic obstruction and the accumulation of a protein-rich interstitial fluid. Chronic inflammation and swelling causes proliferation of fibroblasts and keratinocytes, disruption of normal elastic fibers and the accumulation of subcutaneous lipid deposits. Treatment strategies for lymphedema need to address both facets of this disorder:
1) The acute accumulation of interstitial fluid
2) The chronic adaptive changes
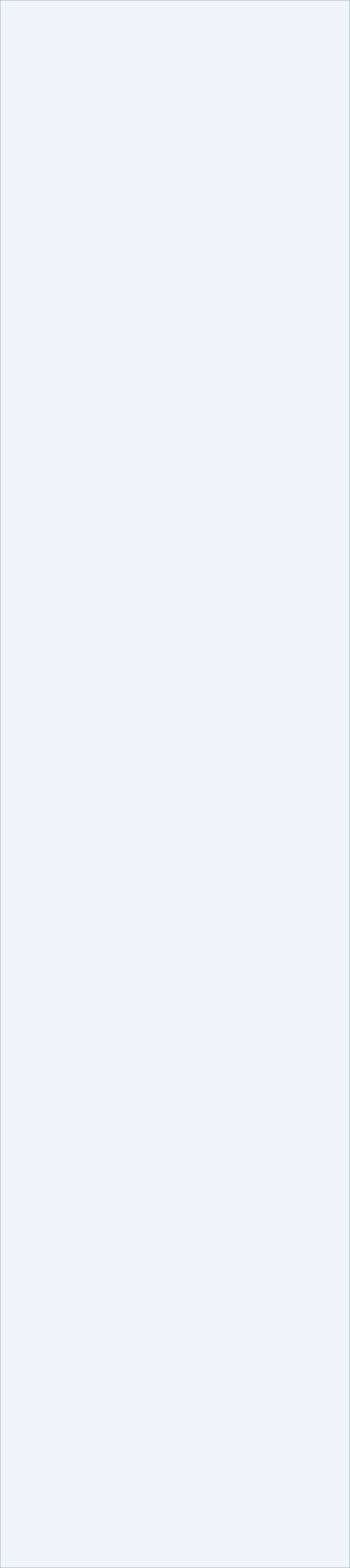
Lymphatic vessels Lymphatic vessels are squeezed by the expansion and recoil of the arterial system contained within the same connective tissue sheath propelling lymphatic fluid forward. Retrograde flow is prevented by numerous one-way valves within the lymphatic vessels. The Optiflow insert dampens the peaks in pressure caused by the pneumatic pumps and maintains a baseline level of compression.
Renee Robinson, Suzie Willis, Cheri Hoskins, Stephen Morgan, Ann Hafner and Tony Reid MD, Ph.D.
Duke University School of Medicine, Healthtronix Lymphedema Management, Inc. and Peninsula BioMedical, Inc.
Abstract
Patients - 35 patients (16 upper extremity/19 lower extremity) with refractory lymphedema were enrolled on a study using the Reid Sleeve in combination with the BioCompression/Optiflow system.
Methods - Patients wore the Reid Sleeve at night. During the daytime, the patients used the BioCompression pump with the Reid Sleeve Optiflow insert for 2 sessions of 60 minutes. Circumferential measurements were made at 3-inch intervals along the length of the arm or leg. The unaffected limb was used as control to determine the percent change from expected except when both limbs were effected.
Results - Among patients with upper extremity edema, the reduction in lymphedema increased steadily during treatment and was 24.7, 53.8 and 80.2% at 4, 12 and 28 weeks. The volume reduction at these times was 2310, 2753 and 4047 cubic centimeters. Linear regression analysis demonstrates a highly significant (p<0.001) reduction in arm edema during the course of treatment. A plateau phase occurred between weeks 4 and 8. For the patients with leg edema, the average reduction at 4 weeks was 9143 cubic centimeters followed by a period of relatively stable lymphedema until week 12 with an average decrease in lymphedema of 1486 cubic centimeters between weeks 12 and 16. Linear regression analysis demonstrates a significant (p<0.02) decrease in leg edema. The plateau phase may represent a tissue repair phase that occurs with effective resolution of residual lymphedema. Subsequent reductions in lymphedema can occur following tissue healing. The plateau phase appears to be more protracted among patients with more serious lymphedema such as patients with leg edema.
Background
Lymphedema is a chronic process due to lymphatic obstruction and the accumulation of a protein-rich interstitial fluid. Chronic inflammation and swelling causes proliferation of fibroblasts and keratinocytes, disruption of normal elastic fibers and the accumulation of subcutaneous lipid deposits. Treatment strategies for lymphedema need to address both facets of this disorder:
1) The acute accumulation of interstitial fluid
2) The chronic adaptive changes
Lymphatic vessels Lymphatic vessels are squeezed by the expansion and recoil of the arterial system contained within the same connective tissue sheath propelling lymphatic fluid forward. Retrograde flow is prevented by numerous one-way valves within the lymphatic vessels. The Optiflow insert dampens the peaks in pressure caused by the pneumatic pumps and maintains a baseline level of compression.
The ReidSleeve utilizes patented technology to provide a gradient of compression within the tissue. Compression is achieved with high and low compression points from resilient but compliant elastic foam, preventing the constriction or tourniquet effect lymphatic venous flow that can occur when compression is applied circumferentially around the arm or leg. The effectiveness of the ReidSleeve has been demonstrated in prior clinical studies.
BioCompression - Intermittent Pneumatic Compression can augment venous and lymphatic flow and is used commonly to prevent deep venous thrombosis among hospitalized patients. Previous randomized studies have demonstrated that intermittent pneumatic compression can help reduce lymphedema.
Rationale for Combination Therapy with ReidSleeve and BioCompression - Intermittent pneumatic compression can prevent static accumulation of venous and lymphatic fluid. The ReidSleeve Optiflow insert can be used inside the pneumatic compression sleeve to further augment venous and lymphatic flow and prevent obstruction due to the tourniquet-effect that can occur with sleeves made of flat, inelastic material. The Optiflow insert dampens the high pressures caused by pneumatic compression and maintains a constant base-line level of compression.
BioCompression - Intermittent Pneumatic Compression can augment venous and lymphatic flow and is used commonly to prevent deep venous thrombosis among hospitalized patients. Previous randomized studies have demonstrated that intermittent pneumatic compression can help reduce lymphedema.
Rationale for Combination Therapy with ReidSleeve and BioCompression - Intermittent pneumatic compression can prevent static accumulation of venous and lymphatic fluid. The ReidSleeve Optiflow insert can be used inside the pneumatic compression sleeve to further augment venous and lymphatic flow and prevent obstruction due to the tourniquet-effect that can occur with sleeves made of flat, inelastic material. The Optiflow insert dampens the high pressures caused by pneumatic compression and maintains a constant base-line level of compression.
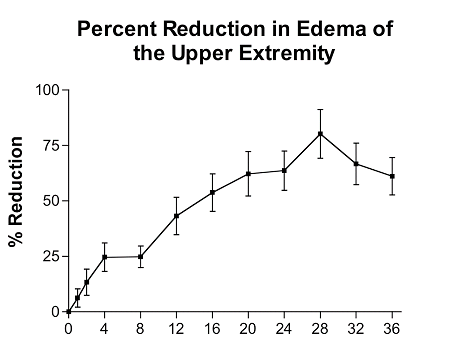
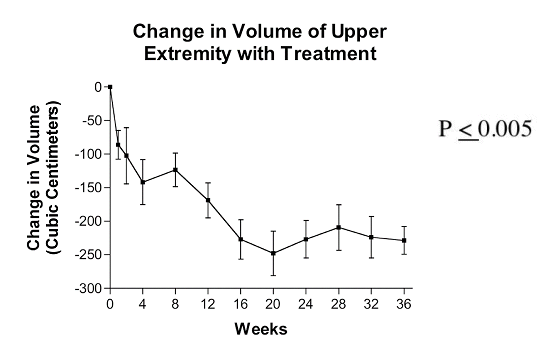
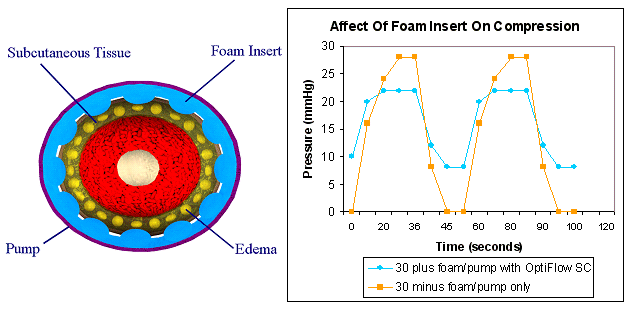
The patients demonstrated rapid and consistent reduction in lymphedema during the first 4 weeks of treatment, achieving a 25% reduction in lymphedema by the 4th week. Between weeks 4 and 8, no significant improvement was observed. Subsequent to week 8, continued reduction was observed. 50% reduction in lymphedema was observed at 16 weeks and 80% reduction was observed at 28 weeks. Between weeks 28 and 36 there is an apparent increase in lymphedema among these patients; however, nearly half of these patients achieved effective control of the lymphedema and entered the maintenance phase of treatment and were seen less frequently. As a result, patients with effectively controlled lymphedema were no longer included at these late time points. Nevertheless, patients with more severe lymphedema were responding and the reduction these patients achieved was 50 to 75% at 36 weeks.
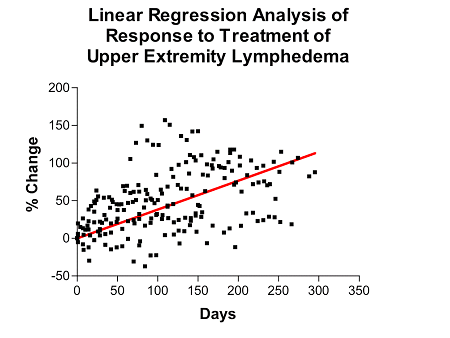
Scattergram of the effect of the ReidSleeve BioCompression/Optiflow System. Linear regression analysis demonstrates progressive decrease in lymphedema with time of treatment.
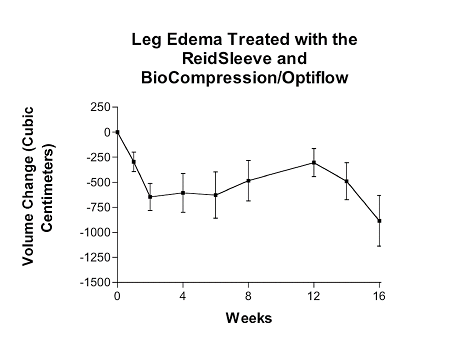
Effect of Combined Treatment with ReidSleeve and BioCompression Optiflow among patients with lower extremity lymphedema. 19 patients with refractory lymphedema were followed for 16 weeks following initiation of treatment using the Duke protocol. The reduction in tissue volume of the affected extremity is shown.
Conclusions
- Response to Treatment: The Reid Sleeve used in combination with the BioCompression/Optiflow system provides effective management for lymphedema of the upper and lower extremity. Patients were followed for up to 1 year of treatment and most patients achieved either complete responses or marked reductions in lymphedema.
- Linear regression analysis: These results demonstrated a strong correlation with clinical response and duration of treatment with optimal results achieved with 3 to 12 months of treatment. The analysis also demonstrates that some patients were transiently worse during the first 1 to 3 months of treatment. This was generally due to infections or other medical issues and patients subsequently responded to treatment after controlling infections of other medical problems.
- Plateau Phase: We observed significant initial reductions in edema are observed within the first few weeks of treatment followed by plateau phase and subsequent secondary phase with further improvement at a slower rate. The plateau phase was longer among patients with lower extremity edema and more severe edema. We hypothesize that free interstitial fluid is readily mobilized with initial treatment but that prolonged and durable responses require tissue healing and that the secondary phase occur s with initial effective management of lymphedema and continued treatment.
Tony Reid MD Ph.D
Dr. Reid's Corner