

 back to Dr. Reid's Corner Directory
back to Dr. Reid's Corner DirectorySentinel Lymph Node Biopsy: Study Update
 email this to a friend
email this to a friend
Several years ago I reported on the use of Sentinel Lymph Node biopsy.. This is a method to accurately assess the presence of metastatic disease that avoids complete axillary lymph node dissection. When I previously summarized the data, there was concern that the technique, while sparing some patients from an axillary dissection, may actually miss some patients with metastatic disease. A recent study further supports the benefit of Sentinel Lymph Node Biopsy.
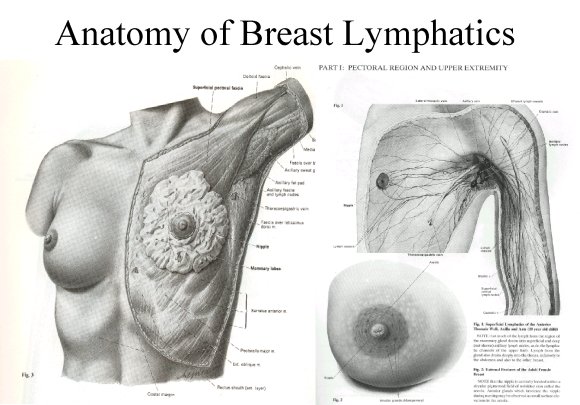
The status of the lymph nodes is the most important single prognostic factor for breast cancer. Cells from cancers of the breast will break off from the cancer and migrate through the lymphatic channels to the regional lymph nodes. As a result, removal of the lymph nodes serves two functions. First, the nodes can be studied under the microscope. If there are no cancer cells in the lymph nodes, the risk of recurrence of the cancer is much lower than if there is metastatic cancer in the lymph nodes and less aggressive treatment is required to control the cancer. Patients with cancer in their lymph nodes will require additional treatment and their chance of recurrence of the cancer is higher. Second, if the cancer does involve the lymph nodes, removal of as much of the cancer as possible is important prior to further treatment with radiation or chemotherapy.
The sentinel node biopsy is an attempt to reduce the extent of surgery required to determine if there is cancer in the nodes. A smaller surgery is likely to lead to fewer complications such as lymphedema.
The lymph nodes are small structures, about the size of a small pea, located throughout the body. They serve as immunological filters to protect the body. Cancer cells from the breast will migrate to the lymph nodes in the axilla. There are over 50 small lymph nodes in the axilla. To determine whether there is cancer in the lymph nodes, a sample of 5 to 10 of these nodes are removed surgically and studied under the microscope. Instead of removing 5 to 10 nodes, the sentinel node biopsy removes the one node most likely to have cancer cells. To do this, a new technique has been developed that uses a combination of a radioactive tracer and a color dye. The dye is injected around the tumor or into the biopsy cavity. The dye will migrate through the lymphatic channels to the regional lymph nodes drained by the cancer. The specific node most likely to be involved with cancer is then identified and removed for microscopic analysis. The important question for the well being of the cancer patient is whether biopsy of one node is sufficient to insure that no cancer cells are missed. It would be a tragedy to allow a woman to die needlessly because an inadequate biopsy resulted in ineffective treatment.
The status of the lymph nodes is the most important single prognostic factor for breast cancer. Cells from cancers of the breast will break off from the cancer and migrate through the lymphatic channels to the regional lymph nodes. As a result, removal of the lymph nodes serves two functions. First, the nodes can be studied under the microscope. If there are no cancer cells in the lymph nodes, the risk of recurrence of the cancer is much lower than if there is metastatic cancer in the lymph nodes and less aggressive treatment is required to control the cancer. Patients with cancer in their lymph nodes will require additional treatment and their chance of recurrence of the cancer is higher. Second, if the cancer does involve the lymph nodes, removal of as much of the cancer as possible is important prior to further treatment with radiation or chemotherapy.
The sentinel node biopsy is an attempt to reduce the extent of surgery required to determine if there is cancer in the nodes. A smaller surgery is likely to lead to fewer complications such as lymphedema.
The lymph nodes are small structures, about the size of a small pea, located throughout the body. They serve as immunological filters to protect the body. Cancer cells from the breast will migrate to the lymph nodes in the axilla. There are over 50 small lymph nodes in the axilla. To determine whether there is cancer in the lymph nodes, a sample of 5 to 10 of these nodes are removed surgically and studied under the microscope. Instead of removing 5 to 10 nodes, the sentinel node biopsy removes the one node most likely to have cancer cells. To do this, a new technique has been developed that uses a combination of a radioactive tracer and a color dye. The dye is injected around the tumor or into the biopsy cavity. The dye will migrate through the lymphatic channels to the regional lymph nodes drained by the cancer. The specific node most likely to be involved with cancer is then identified and removed for microscopic analysis. The important question for the well being of the cancer patient is whether biopsy of one node is sufficient to insure that no cancer cells are missed. It would be a tragedy to allow a woman to die needlessly because an inadequate biopsy resulted in ineffective treatment.
A recent study followed 971 patients who had sentinel lymph node biopsies and were found to be free of cancer. The important question was how many of these women had residual breast cancer that was missed by the sentinel biopsy. These patients have been followed for an average of about 2 years and many for 4 years or more.
The study was divided into two phases. In the first phase, 120 women who has sentinel node biopsies and were found to be free of disease subsequently underwent the standard lymph node dissection. Residual disease was found in one woman. Thus, the sentinel node biopsy is slightly better than 99% predictive of whether there is cancer in the axillary lymph nodes. In the second phase of the study, 971 women underwent sentinel lymph node biopsy and if they were free of disease did not have additional axillary dissection. Instead, they were observed. To date, there have been no recurrent cancers in the women who were found to be negative on the sentinel node biopsy. The recurrence of breast cancer usually happens within 5 years of the initial diagnosis and about 75% become evident in the first 2 to 3 years. About half of the women in the study have reached the 2 year point after the sentinel node biopsy, so the data are very encouraging at this point. However, additional time is needed to be assured that these women will remain free of disease.
The study also reported that the extent of edema immediately following the surgery was less in the patients undergoing sentinel lymph node biopsy compared to the women undergoing traditional axillary dissection. They also noted that fewer women experienced arm numbness in the period after the surgery. Since lymphedema can occur many years after the surgery, it is still too early to tell what the rate of lymphedema will be in women undergoing sentinel lymph node dissection. However, it is very likely that the rate of lymphedema will decrease with sentinel lymph node dissection. Since these women still undergo radiation to the axilla, the rate of lymphedema may not drop to zero, but I think that the sentinel lymph node biopsy is very likely to significantly decrease the incidence of lymphedema. I expect further data on this study in the next few years and will keep you updated on the results.
I have been very pleased with the number of very positive responses we have received since starting the Lymphedema Chronicles. Many people have felt that this was a welcome forum to express their feelings and experiences with lymphedema. Many more people have expressed their appreciation for the valuable insights and information they have received from reading these chronicles. I would like to expand on the format of the Lymphedema Chronicles. One of my patients found that art work was very helpful therapy for her. She created beautiful drawings as well as collages of pictures that described her feelings and state of mind as she went through treatment for breast cancer. I had another patient who wrote short stories describing her experiences. If anyone wishes to share their creative nature as part of the Chronicles, you may send your story or an image of your art work along with your Chronicle.
Tony Reid MD Ph.D
The study was divided into two phases. In the first phase, 120 women who has sentinel node biopsies and were found to be free of disease subsequently underwent the standard lymph node dissection. Residual disease was found in one woman. Thus, the sentinel node biopsy is slightly better than 99% predictive of whether there is cancer in the axillary lymph nodes. In the second phase of the study, 971 women underwent sentinel lymph node biopsy and if they were free of disease did not have additional axillary dissection. Instead, they were observed. To date, there have been no recurrent cancers in the women who were found to be negative on the sentinel node biopsy. The recurrence of breast cancer usually happens within 5 years of the initial diagnosis and about 75% become evident in the first 2 to 3 years. About half of the women in the study have reached the 2 year point after the sentinel node biopsy, so the data are very encouraging at this point. However, additional time is needed to be assured that these women will remain free of disease.
The study also reported that the extent of edema immediately following the surgery was less in the patients undergoing sentinel lymph node biopsy compared to the women undergoing traditional axillary dissection. They also noted that fewer women experienced arm numbness in the period after the surgery. Since lymphedema can occur many years after the surgery, it is still too early to tell what the rate of lymphedema will be in women undergoing sentinel lymph node dissection. However, it is very likely that the rate of lymphedema will decrease with sentinel lymph node dissection. Since these women still undergo radiation to the axilla, the rate of lymphedema may not drop to zero, but I think that the sentinel lymph node biopsy is very likely to significantly decrease the incidence of lymphedema. I expect further data on this study in the next few years and will keep you updated on the results.
I have been very pleased with the number of very positive responses we have received since starting the Lymphedema Chronicles. Many people have felt that this was a welcome forum to express their feelings and experiences with lymphedema. Many more people have expressed their appreciation for the valuable insights and information they have received from reading these chronicles. I would like to expand on the format of the Lymphedema Chronicles. One of my patients found that art work was very helpful therapy for her. She created beautiful drawings as well as collages of pictures that described her feelings and state of mind as she went through treatment for breast cancer. I had another patient who wrote short stories describing her experiences. If anyone wishes to share their creative nature as part of the Chronicles, you may send your story or an image of your art work along with your Chronicle.
Tony Reid MD Ph.D
Dr. Reid's Corner